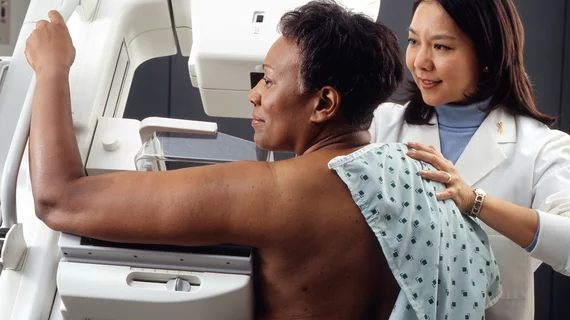
When primary care physicians (PCP) interact with their patients at a high level, it leads to improvements in breast cancer screening adherence for all racial and ethnic minority groups, according to new findings published in the Journal of the American College of Radiology.
“As the United States continues to become increasingly diverse, understanding factors that affect access to routine screening mammography is an important step in improving breast cancer disparities among racial/ethnic minority groups,” wrote Efrén J. Flores, MD, department of radiology at Massachusetts General Hospital in Boston, and colleagues. “Therefore, the purpose of this study was to determine the association between interactions with primary care physicians and adherence to recommended screening mammography guidelines across different racial/ethnic groups over a 10-year period.”
The authors tracked data from patients between the ages of 50 and 64 who underwent screening mammography in 2005 at a single institution. Each patient’s adherence to mammography recommendations was noted at two-year intervals for 10 years. The team also used electronic medical records to determine which patients had a high level of PCP interaction.
Overall, more than 9,000 patients were included in the study, and they underwent more than 71,000 mammograms during the study. Looking at the group’s demographics, 84.5 percent of the patients were white, and more than 97 percent were insured by either private insurance or Medicare. More than 37 percent had high levels of PCP interaction.
During the study period, more than 71 percent of women missed at least one screening examination. This included more than 71 percent of white women, more than 68 percent of black women, more than 64 percent of Hispanic women, more than 70 percent of Asian women and more than 71 percent of women who identified as “other.”
Patients with high PCP interaction had increased adherence to recommended screening mammography guidelines across the board. The improvement was noted in black patients, Hispanic patients, Asian patients and patients who identified as “other.”
“High PCP interaction was associated with improved screening mammography adherence for women of all races,” the authors wrote. “Although previous studies have found that PCP visits are associated with greater use of mammography and lower breast cancer mortality, these studies were not stratified to evaluate this effect across different demographics.”
The team also noted that Medicaid and self-pay or other insurance categories were associated with lower screening adherence compared to patients with private insurance.
“Although screening mammography is a service covered under Medicaid with no additional cost to the patient, patient participants of Medicaid services encounter other structural barriers when accessing health care services,” the authors wrote. “Patients with Medicaid are less likely to be offered appointments for diagnostic imaging services compared with Medicare patients, potentially because of lower reimbursement rates compared with Medicare or private insurance. Consequently, Medicaid enrollees are also more likely to present with advanced-stage breast cancer.”